Alameda County Health Clinic Network for Neediest
Resource type: News
San Francisco Chronicle | [ View Original Source (opens in new window) ]

By Stephanie M. Lee
Getting blood drawn should have been an easy part of Selesi Alatini’s checkup. But on this day, the nurses at Havenscourt Health Center in East Oakland were struggling to find a vein in her arm.
“I don’t really see anything that I’m comfortable about,” Karen Gersten-Rothenberg, a nurse practitioner, told the 16-year-old high school senior. “How hard is it for you to come back?”
Not hard at all.
The school Selesi attends, Coliseum College Prep Academy, is just a few steps from Havenscourt, one of dozens of community clinics set up to offer affordable health care to hundreds of thousands of low-income and underinsured people in Alameda County.
The county has about 70 of these clinics. Twenty-eight of them treat students on school campuses. Others serve the homeless and chronically ill. Havenscourt is one of the newest. No mere nurse’s office, it provides physical, reproductive and mental health care to students at both Coliseum College Prep and Roots International Academy, an adjoining middle school.

Clinics like these began emerging in Alameda County in the 1970s. But some of the more recent ones were the result of an expansion by public health leaders who found inspiration in a surprising place: Cuba.
Between 2008 and 2010, Alameda County officials and public health providers traveled to the island nation to study nationalized health care – a system that spends relatively little, but emphasizes primary and preventative care, and enjoys low infant mortality, long life expectancies and other measures of strong health.
Cuba’s influence
Back home, they tried to combine what they saw with the public health services they had in place. They wanted their local clinics to be places where doctors treat patients holistically and where patients aren’t afraid to take charge of their health.
In the United States, the traditional attitude toward health care is: “Wait your turn, do what the doctor says,” said Alex Briscoe, director of the county’s Health Care Services Agency.
“What Cuba and other progressive health systems do is focus on patient empowerment and education,” he said. “How do we engage more effectively our patients in their own care?”
Havenscourt clinic
A few minutes in Havenscourt’s waiting room offer a glimpse of the kind of health care that Briscoe is talking about.
Located at 66th Avenue and International Boulevard in Oakland, the center serves 800 students at Coliseum College Prep, which serves sixth through 12th grade, and Roots International Academy middle school.

Off campus, the neighborhood has a history of gang activity and violence, and low-income housing projects line the streets. On campus, suspensions and disobedience are common.
“Adolescents are typically physically the healthiest age cohort,” said Gersten-Rothenberg, the clinic’s supervisor. “But we uncover a tremendous amount of trauma.”
Opened in November 2011 in the rent-free, renovated space of a former woodshop, the office is full of light, colorful posters and smiling, Spanish- and English-speaking staff. Most students are Latino, and one-fifth are African American. The half-dozen staff members there at any one time try to keep the atmosphere welcoming and safe for students.
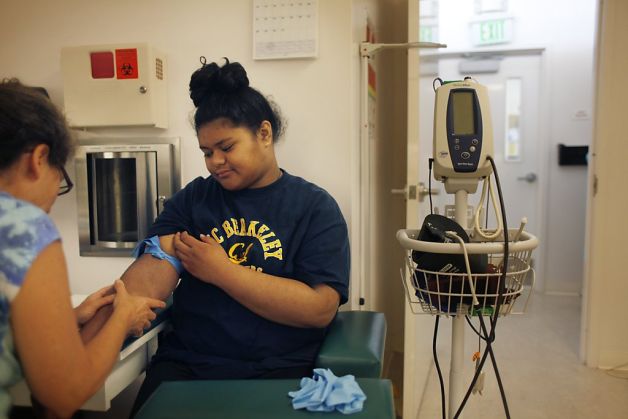
Even during summer school this year, teens arrived for physical exams, dental checkups and counseling appointments. More than 30 patients come by every day.
Selesi, the high school senior getting her blood drawn, had previously dropped in for flu shots and chats with a health counselor during sanctioned class breaks. If she wanted, she could get birth control, immunizations and a dentist appointment.
“You can come here for everything,” she said.
Some patients arrive with parents, others come alone. Most are current students, but the clinic accepts alumni and students who have transferred to schools elsewhere until age 21. For some, it is one of the few places where they can reliably get care.
No one turned away
On a recent morning, Erika Muniz brought her 10-year-old son and 11-year-old daughter for checkups. The housekeeper said she and her husband, a house painter, cannot afford health insurance. “We don’t have the jobs to be able to,” she said in Spanish.
Half of the clinic’s patients are on Medi-Cal; the rest are uninsured or insured through the county or private providers. No one is turned away.
At the center, which is run by La Clínica de La Raza, 75 percent of the $500,000 budget comes from reimbursements for Medi-Cal and other services. The rest is a mix of grants and government funds. So the staff works hard to sign up students for insurance.
In a recent UCSF survey of students who used the county’s school-based clinics, nearly all said they had learned to eat better, exercise more and use contraception more consistently. For many, the centers fill a need: One-third lacked regular primary care.
Nearly 2,000 school health centers exist nationwide. Studies find that students who use them show improved attendance rates and grade point averages compared with their peers, and have fewer emergency-room visits.
Havenscourt takes primary care a step further by inviting teens to be proactive about their well-being. It trains a team of students to give class presentations about health, and encourages patients to tell their friends about the clinic.
“We’re giving our kids opportunities to get care on their own, be responsible for doing whatever they’re doing or not doing in their lives,” Gersten-Rothenberg said.
But failure to show up for an appointment will be quickly followed with a call to the student’s home or class.
“We go find the students, and if they’re not in school today, we reschedule them for tomorrow,” Gersten-Rothenberg said. “And if they’re not in school tomorrow, we reschedule them for next week.”
By getting them to take responsibility for their own care, she said, “we’re more Cuba than the United States.”
Lessons from Cuba
Cuba, a nation of 11 million people, may seem an unlikely source of inspiration. Critics of the communist state – including the U.S. – condemn its severe limits on speech and religion.
In terms of quality of health care, however, it rivals many developed nations. A Cuban’s life expectancy is 78, while an American’s is 79. Cuba’s infant mortality rate is 4.76 deaths per 1,000 live births, while the United States’ is 5.9. Cuba also has the lowest AIDS prevalence rate in the Americas.
These achievements are in spite of relatively low health care expenses – $430 per person compared with $8,600 in the U.S.
And those achievements inspired the Oakland nonprofit Medical Education Cooperation with Cuba, or Medicc, 15 years ago to organize research and educational visits by U.S. health professionals.

“I don’t want to imply Cuba has all the answers, because there’s vast differences in political and social structures between Cuba and us,” said Diane Appelbaum, Medicc’s U.S. director. “Even with the differences, I think Cuba’s system can provide some important cost-effective and evidence-based examples we can learn from.”
From 2008 to 2010, more than 40 people from a dozen Bay Area organizations traveled to Havana. They included Wright Lassiter, CEO of Alameda Health System, which treats thousands of chronically ill patients.
In March 2010, Lassiter learned there are thousands of clinics in Cuba, each serving 600 people in their neighborhoods, where the physicians and nurses also live. These clinics address 80 percent of their patients’ health problems, provide primary care services like immunizations, and refer patients with greater needs to specialty clinics. Hospitals are the last stop.
Because of this extensive network – as well as the government’s ability to afford many doctors by paying them low wages by international standards – the nation has one of the world’s highest doctor-to-patient ratios: 67.2 to 10,000.
Knowing their patients
Lassiter knows that the U.S. can’t replicate that model exactly. But inside weathered concrete buildings, he found clinics operating with basic medical tools and doctors who knew their patients inside and out. That appealed to him.
“You walk into a doctor’s office, there’s a family medical record for every patient taken care of,” he recalled. “He or she knows the maladies your grandmother had and has been thinking about your health in the context of a familial health environment, but without computers.”
Lassiter was especially struck by the way the system was set up to distinguish between patients with regular needs and those who needed more help than one doctor could give.
In January, he helped open the Hope Center in Oakland to serve patients who have been hospitalized three or more times in the past year. The goal is to reduce their hospitalizations by assigning them a medical director, social worker and nurse care managers to oversee prescriptions, arrange appointments and check on patients at home.
So far, the office has treated more than 80 people. Patients report better physical and mental health after three months there.
“When it comes to health, coming to the clinic is really only a small part of it,” said Dr. David Moskowitz, the medical director. “By addressing health more broadly, we’re able to meet patients where they’re at and hopefully intervene a little bit more effectively.”

A source for doctors
In Cuba, Lassiter was also impressed by students he saw at the Latin American School of Medicine, which educates aspiring doctors from all over the world for free.
Watching American residents there make hospital rounds speaking fluent Spanish, Lassiter thought perhaps they could help many of his Spanish-speaking Latino patients.
So for three years, with Medicc’s help, 31 students from the school have done summer rotations in Alameda County clinics and hospitals.
Maiti Rodriguez, 28, just interned at Kaiser Permanente in Fremont and Hayward, and helped patients in Spanish. Drawn to the idea of an education abroad, the Oakland native wants to practice family medicine in the Bay Area – with the personal approach to patients that she learned in Cuba.
“We’ve become so used to sending for labs and tests and stuff like that, it’s become normal,” she said. “The basics are what we really need. Asking questions, interviewing patients, doing a physical exam – people say that that’s 90 percent of diagnoses.”
In the view of Alameda County’s health leaders, school-based centers such as Havenscourt have done well since they opened. The network of community clinics they belong to has also been thriving. The foundation had already been laid, but Cuba reinforced their sense that this method worked.
“Mix them all together,” Briscoe said of the different sources of ideas, “and we think we’re on to something.”
Since the Cuba trips, nine school health centers have opened. Four more are planned in Oakland, Hayward, San Leandro and Emeryville.
New medical center
Health officials have teamed with Oakland and Hayward centers for day laborers and immigrants to provide on-site medical care and connect patients to health care options. In Hayward, a new medical center is planned to open next door to a fire station.
And at another location in Oakland, the new Trust Clinic is geared toward patients who are homeless, disabled and on welfare. The plan is to have doctors, nurse practitioners and mental health workers on site. Lawyers and case managers will help patients find housing, and tap into Social Security and disability benefits.
Director Wendy Georges calls the clinic the “safety net for the safety net.”
“We decided the only plausible, sensible approach to take would be to bring all of the services that that population needs under one roof,” she said.
Oakland won’t turn into Havana any time soon. But Alameda County leaders hope American health care will improve as the Affordable Care Act attempts to emulate some of the best qualities of that nation’s system.
The health law is pouring billions of dollars into programs to prevent chronic diseases, enabling community clinics to expand. Volunteers are being trained to help people sign up for insurance and penalties will be imposed on hospitals with high rates of repeat patients.
‘Unified system’ needed
“There’s a lot of great community organizations in our country, but I think the (law) also has recognized that they need to be brought in more to a unified system to be more effective,” said Appelbaum, whose group has also organized research programs in Cuba for medical workers from Los Angeles and New Mexico, and invited Cuban health workers to the United States.
Another crucial goal of the law is to enroll low-income people in Medicaid, possibly one of its most difficult tasks. So it’s critical for medical centers to reach out to those patients, Briscoe said.
“It doesn’t matter how good a clinic you are if your patients don’t show,” he said.
At Havenscourt, Selesi Alatini is one patient who takes pride in getting to her appointments. After failing to get her blood drawn, she returned and succeeded. Then she got her teeth checked, and signed up for a teeth cleaning.
“You can just walk in yourself,” she said. “And you’re doing things on your own.”
Learn more about Alameda County’s clinics at http://www.alamedahealthconsortium.org/.
This project was produced for the California Endowment Health Journalism Fellowships (ReportingonHealth.org), a program of USC Annenberg’s School of Journalism. Stephanie M. Lee is a San Francisco Chronicle staff writer.
Havenscourt Health Center is part of Elev8, a program providing school-based health care and community support to middle school students and their families. View a complete list of Atlantic’s Elev8 grantees >
To Learn More about Elev8:
> Visit our Elev8 page for videos and updates
> Visit www.elev8kids.org or the websites of the local initiatives:
Elev8 Baltimore
Elev8 Chicago
Elev8 New Mexico
Elev8 Oakland
Elev8 is a grantee of Atlantic’s Children & Youth programme in the United States, which funds efforts to support and expand community schools.
